|
11 The analysis was restricted to patients who were enrolled in fee-for-service Medicare, aged ≥ 66 years. 15, 16 Results from this database are made available to consumers on CMS’ Hospital Compare website, aggregated at the hospital level. It contains patient-level data, including quality of care assessments using uniform instructions, principal and secondary diagnoses, procedures performed, discharge disposition status, the patient’s ZIP code of residence, age, gender and reported race/ethnicity. 
We used the Quality Improvement Organization (QIO) Clinical Data Warehouse (CDW), which is an electronic database currently being used by CMS for the Hospital IQR Program, The Joint Commission, and the Hospital Quality Alliance (HQA) initiative. We performed a cross-sectional analysis using discharge and quality of care assessment records that were submitted by hospitals that participated in the Hospital Inpatient Quality Reporting (IQR) Program 11, 15 from January 1 through December 1, 2007. 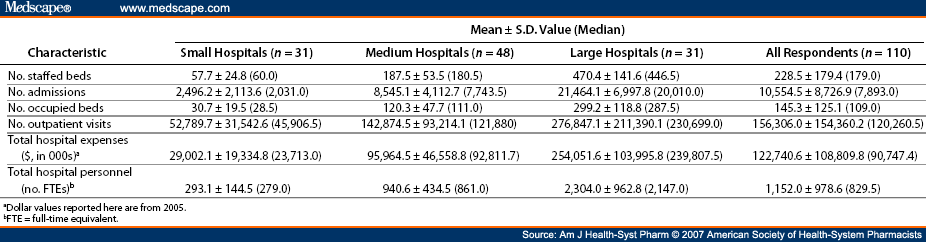
We explored the relationship between hospital performance on Medicare’s Hospital Compare process quality measures and risk-standardized all-cause 30-day readmission rates for patients aged 66 or older, with a principal discharge diagnosis of acute myocardial infarction (AMI), heart failure (HF), or pneumonia, or undergoing abdominal, cardiac and vascular, or orthopedic surgery. These process measures focus on appropriate medications at the time of discharge, vaccination, and discharge instructions, and hospitals that are more successful at delivering such interventions might experience lower readmission rates. While previous studies have observed only a weak association between performance on these process measures and 30-day mortality rates, 12 – 14 it is possible that these interventions have a greater effect on readmission than on mortality. Little is known, however, about whether greater adherence to the process of care quality measures reported on the Centers for Medicare & Medicaid Services (CMS) Hospital Compare website 11 is associated with lower readmission risk. Earlier studies, 7, 8 as well as more recent single-institution analyses, 9, 10 have suggested that better quality of inpatient care is associated with a lower risk of readmission. 5, 6 The large clinical impact, coupled with growing concerns about current levels of health care spending, has made reducing readmission rates a national priority and a central goal of health care reform legislation.Įxisting literature on the association between hospital care processes and outcomes have provided inconsistent results. Within 30 days of discharge, as many as one in four patients will return to the hospital, 1 – 5 and it has been estimated that unplanned readmissions were responsible for $17.6 billion in Medicare spending in 2004. 
Hospital readmissions are common, potentially harmful for patients, and enormously costly to the US health care system.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
